with our monthly newsletter.
To curb the spread of COVID-19 and emerging variants globally, we need to ensure fair, equitable access to vaccines. To date, supply shortfalls and delayed shipments have led to the slow roll out of vaccines. Guatemala, for example, has one of the lowest vaccination rates in Latin America, with only 3.5 doses administered per 100 population. Though Guatemala is poised to receive additional vaccine supplies (including a donation of 1.5 million doses of the Moderna COVID-19 vaccine by the United States Government in July), there are additional barriers getting doses into arms once shipments arrive in countries.
Guatemala has struggled with the cold chain requirements of certain vaccines, ensuring adequate human resources for administering vaccines, setting up accessible systems to register people for vaccine appointments, and countering vaccine misinformation and hesitancy.
While most low- and middle-income countries have national deployment and vaccination plans that identify priority population groups, inconsistent supply may call for on-the-fly strategy adaptations based on changes in timing and availability of specific vaccines. Additionally, countries need information to operationalise these plans to distribute doses quickly in an equitable way, prioritising vaccines to those most adversely impacted by COVID-19 and ensuring equal access, particularly amongst vulnerable populations, to guarantee high vaccine uptake.
So, where does data come into play?
Country governments need tools that can quickly use available data to inform these decisions and help understand the impact of different allocation choices. In partnership with the technology company Fraym, Palladium worked with country implementers in Guatemala to identify and adapt tools to inform decisions on where to prioritise vaccine rollout and plan vaccination delivery strategies.
First, how can governments use available data to inform planning and prioritisation of limited vaccines?
To address this question, Palladium applied their VaxImpact model, an epidemiological model that estimates the health and mortality impacts of vaccine allocations to population subgroups and geographic areas. The team considered three different vaccine distribution strategies, which prioritised vaccines to municipalities in Guatemala based on the number of people in the highest-risk age group (ages 70+), COVID-19 deaths per capita, or a vulnerability score generated by Fraym.
The vulnerability score for each municipality reflects several COVID-19 risk factors including rates of pre-existing conditions, access to media, coverage of other vaccines, and age. For each scenario, the model projected COVID-19 cases and deaths through the end of 2021.
The model results show that with Guatemala’s 20 percent target for vaccine coverage in 2021, municipalities with high densities of older people should continue to be prioritised, as they are at far higher risk of COVID-19 mortality. Interestingly, changing the geographic prioritisation of vaccines based on mortality alone, or vulnerability, had only a small impact on national COVID-19 cases and deaths, because the difference in COVID-19 mortality across larger geographic areas is much smaller than the difference between age groups. If there were more variability across municipalities, there may have been a larger impact. In addition, the three strategies used in the model to allocate vaccines resulted in the prioritisation of similar municipalities in each scenario.
Second, how can countries operationalise vaccination delivery strategies to reach individuals most at-risk for COVID-19?
Once specific municipalities are prioritised for vaccination using the VaxImpact model, hyper-local heat maps can be used to help immunisation program managers ensure successful delivery of COVID-19 vaccines to high-incidence communities. In the context of limited vaccine supply, precise targeting of vaccines to the right populations in the right geographies can reduce wastage.
Fraym used advanced machine learning models that combine population-based survey data, administrative data, remote sensing data, and satellite imagery to derive insights to inform vaccine microplanning in Guatemala.
Using these hyper-local maps, priority populations (e.g., adults over age 70) can be mapped at the 1 km2 level across the country, indicating where and how many elderly individuals reside in specific locations to inform day-to-day planning and allocation of vaccine doses. This information, paired with other health and socioeconomic data, can further identify those who may be more at-risk for adverse COVID-19 outcomes and tailor vaccination delivery strategies to reach these vulnerable populations.
For instance, the maps can help to identify communities with large numbers of elderly populations in areas with poor access to health facilities and plan vaccination strategies such as the deployment of mobile vaccination teams and staff to directly reach these individuals.
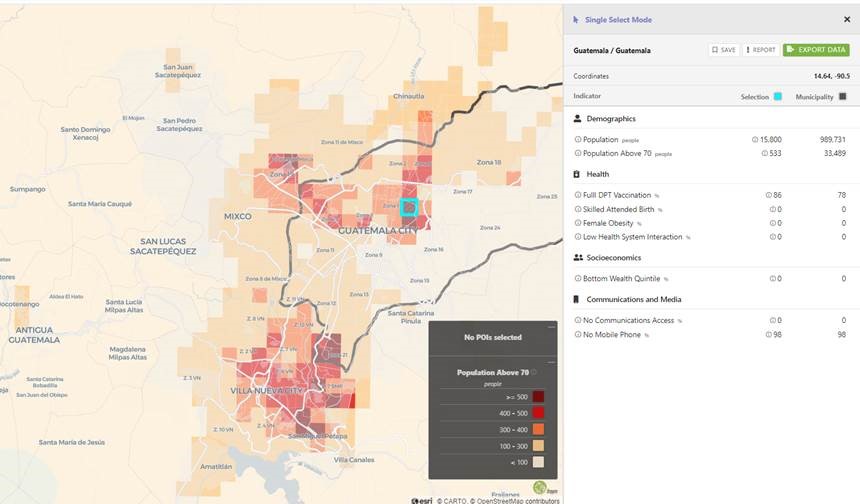
Further analysis of this data can reveal insights into contextual factors that might impact demand and uptake for vaccines. Previous immunisation behaviours can be analysed to understand which communities might be under-vaccinated and potential reasons behind vaccine hesitancy. Pairing this information with communications consumption data, program managers can design community mobilisation and social and behaviour change interventions tailored to reach these specific populations.
In addition to supply constraints, countries are grappling with logistics challenges, vaccine hesitancy, and misinformation, which impede vaccine roll-out. Models and comprehensive local information that make use of already existing data can help decision-makers prioritise geographies, understand where and how to reach individuals, and plan interventions to increase acceptance and uptake of vaccines. The right analytic tools, combined with good data, can help countries reach high-risk and vulnerable populations, mitigating the health and mortality impacts of COVID-19.
Learn more about Palladium’s VaxImpact Model or Fraym’s Equitable Vaccine Allocation Model. For more information contact info@thepalladiumgroup.com.
with our monthly newsletter.

